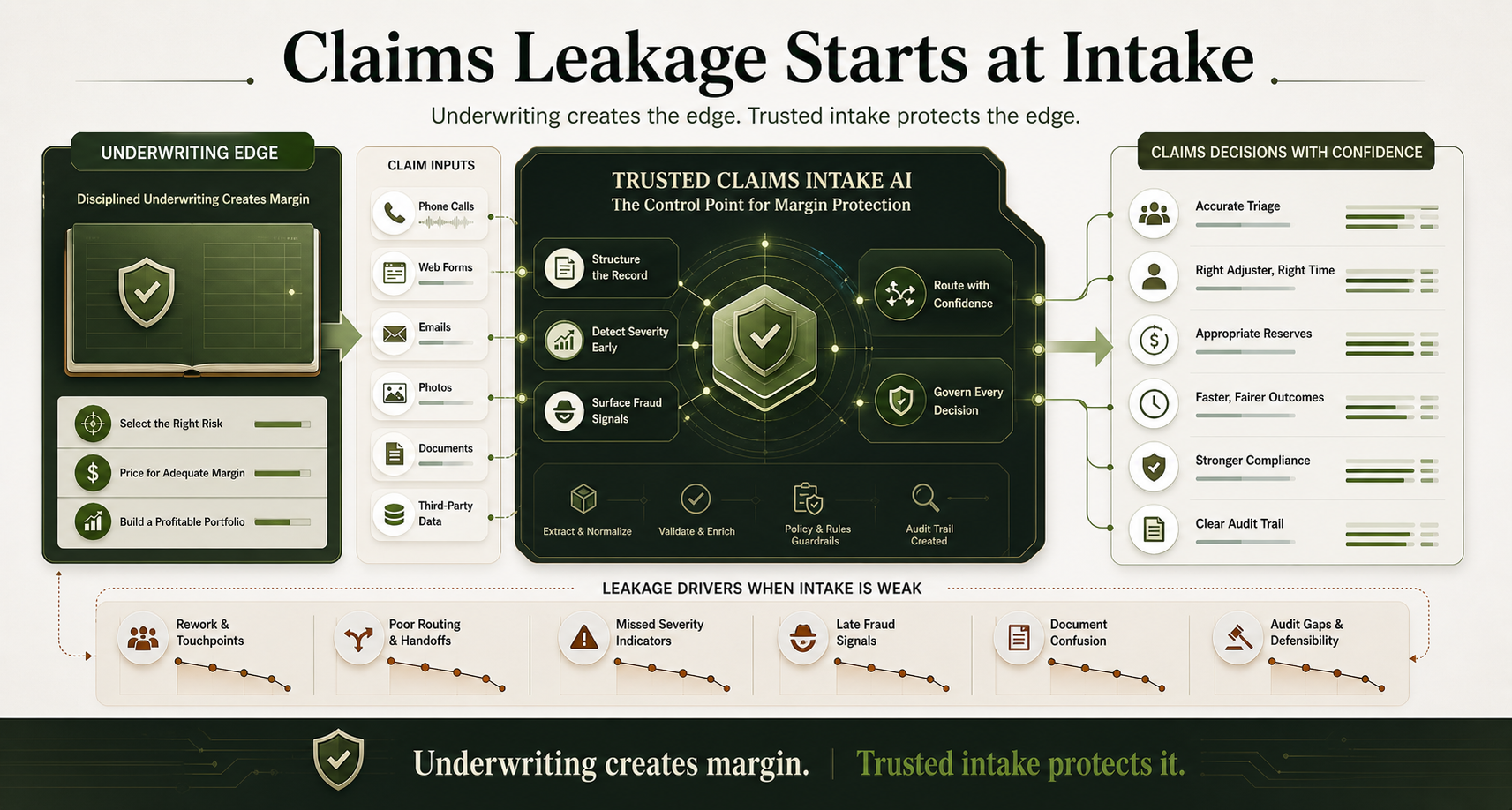
Underwriting Wins the Business. Bad Claims Intake Gives the Margin Back.
The next edge in P&C insurance won't come from pricing alone; it will come from Trusted Claims Intake AI that stops leakage before it enters the claim file.
Underwriting Creates the Advantage. Claims Decides Whether You Keep It.
Insurance leaders spend enormous energy sharpening underwriting. Better data, better models, better segmentation, better pricing discipline, better portfolio steering. That work matters. Underwriting is where the carrier chooses the risk, shapes the book, and earns the right to compete.
But there is a quieter truth inside many P&C operating models: underwriting may create the edge, but claims often determines how much of that edge survives.
Not because claims teams are careless. Not because adjusters lack judgment. Not because carriers have ignored claims transformation. The problem is more structural than that. Too many claims operations are built around fixing claims problems after bad intake already happened.
That worldview is the leak.
A claim enters through a call, a web form, an email, a photo set, a police report, a repair estimate, a medical bill, a handwritten note, or a broker submission. The first version of the claim record is assembled under pressure, often across fragmented channels, incomplete fields, inconsistent documents, and unstructured narratives. Then downstream teams are expected to triage accurately, assign correctly, detect severity, surface fraud signals, comply with governance rules, and make confident decisions from a file that was never trusted at the start.
The Expensive Myth of Downstream-First Claims Transformation
For years, the industry has tried to improve claims by adding intelligence later in the workflow. Better dashboards. Better litigation analytics. Better payment controls. Better adjuster workbenches. Better document repositories. Better reporting. All useful. None sufficient.
The reason is simple: if the claim record is weak at intake, every downstream system inherits the weakness. Triage becomes guesswork wrapped in workflow. Routing becomes a rules engine fed by partial facts. Fraud detection becomes retrospective pattern matching instead of early signal recognition. Governance becomes a review layer added after decisions have already started moving. Adjusters spend their first hours cleaning the file instead of advancing the claim.
This is how leakage becomes normal. Not dramatic leakage. Not the kind that announces itself in a board deck. The everyday kind: duplicate work, missed severity cues, avoidable handoffs, late specialist assignment, poor documentation, inconsistent coverage context, unstructured attachments, audit gaps, and decisions made with too little confidence too late in the process.
The villain is not legacy software. The villain is the belief that carriers can compensate for untrusted intake by becoming more efficient downstream.
That belief is getting expensive.
Claims Intake Is Not Administration. It Is the Control Point.
The first notice of loss is often treated as the beginning of a process. Operationally, it is much more important than that. FNOL and claims intake are the control point where the quality of the claim record is created.
At intake, the carrier has the first opportunity to capture the facts, structure the narrative, validate the information, extract document data, detect missing evidence, surface risk signals, identify severity, determine complexity, and route the claim to the right path. Once that opportunity is missed, the organization spends the rest of the claim trying to reconstruct what should have been captured correctly at the beginning.
This is why the intake layer deserves a category of its own. Not generic AI for insurance. Not another claims automation widget. Trusted Claims Intake AI.
Trusted Claims Intake AI is the operating layer that turns the chaotic first moments of a claim into a governed, structured, explainable claim record. It does not replace claims judgment. It prepares the ground so human judgment starts from a cleaner, more reliable position.
Trusted Claims Intake AI Is a Governance Strategy
The word trusted is not decorative. In claims, trust is operational.
A claims AI system that cannot explain what it extracted, what it flagged, what it masked, what it routed, and why it recommended the next action is not ready for serious claims operations. Claims decisions affect customers, reserves, litigation risk, regulatory posture, and brand reputation. Governance cannot be bolted on after automation has already influenced the file.
Trusted Claims Intake AI starts with governance inside the intake layer: PII detection, masking, policy gates, bias monitoring, decision explainability, regulatory alignment, and a full audit trail. It makes the early claim record not only more useful, but more reviewable.
This is the difference between speed and confidence. Speed alone can move bad information faster. Confidence means the organization knows what came in, how it was interpreted, what signals were present, what was uncertain, and what needs human review.
The Future Belongs to Carriers That Trust the File Earlier
The next era of claims performance will not be won only by carriers with better underwriting models. Underwriting will remain essential, but the carriers that protect the margin will be the ones that stop letting claim quality leak at the front door.
The future claims operation looks different. The claim record is trusted before assignment. Documents are extracted and structured before review. Fraud and severity signals surface at intake. Routing is based on complexity, exposure, and evidence rather than incomplete categories. Adjusters begin with context instead of cleanup. Governance is native, not reactive. Leaders can see why a claim moved the way it moved.
The market is moving from downstream-first claims automation to upstream claims trust. Once that shift becomes obvious, neutrality disappears. A carrier is either early to the intake layer or late to the leak.